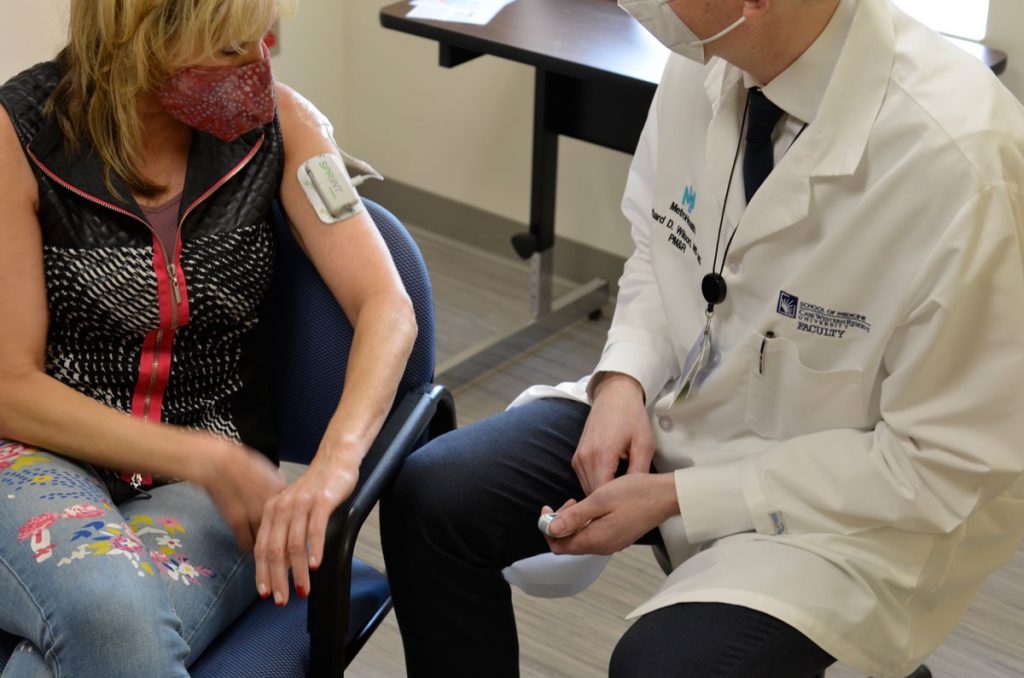
Seven weeks of electrical stimulation provided transformative results. “It’s wonderful,” Riccio says, adding that she again can wash and condition her hair on her own.
Riccio’s story illustrates the benefits of Wilson’s research into alleviating chronic shoulder pain via an FDA-approved electrode implanted under the skin.
Wilson’s work is one part of the ongoing research taking place through the FES Center, a consortium of five nationally recognized institutions: Louis Stokes Cleveland VA Medical Center, Case Western Reserve University, MetroHealth Medical Center, University Hospitals, and Cleveland Clinic Neurological Institute.

Researchers, engineers and clinicians collaborate to develop innovative solutions that improve quality of life for individuals with neurological or musculoskeletal impairments.
Riccio found Wilson’s study while searching online after therapy disruptions during COVID. She applied, was accepted, and agreed to a short implantation procedure.
In September, a few weeks into stimulation and follow-up therapy, she reached for her phone without pain. “This is such a relief,” she says.
“One hundred percent,” she says when asked if she would recommend the treatment.
Wilson’s is one approach among several FES pain projects: muscle stimulation, direct-current nerve blocking, and mapping neural pain pathways in the brain.
Blocking a nerve to block pain
Tina Vrabec, PhD, is developing tiny cuff electrodes that attach to specific nerves. When direct current runs through the electrode, nerve firing can be blocked and chronic pain may be relieved.
Her goal is a controllable, non-addictive option. In her model, patients could control the level of block via an external device with localized effects and instant on/off behavior.
Vrabec’s work is currently pre-clinical and examines implanted, percutaneous, and external electrode approaches.
She aims for clinical trials in the next few years and eventual FDA approval for chronic pain conditions such as lower back pain and migraines.

Mapping pain circuits in the brain
Carl Saab, PhD, leads the Pain STAR Lab at Cleveland Clinic and studies how chronic pain is represented in brain circuits.
His team uses optogenetics in pre-clinical work to map neural pathways with high precision and identify sensory circuits that misbehave during pain.
Saab believes future pain treatment should be guided by brain network data, potentially enabling objective diagnostics and more targeted therapies.


Electrical stimulation to fight pain
Wilson is more than a decade into stimulation-based pain research and is running clinical trials to understand long-term outcomes, responder profiles, and combinations with physical therapy.
The implanted electrode stimulation is typically barely noticeable and allows participants to continue normal daily activity while treatment is delivered.
Wilson sees potential expansion to lower back pain, knee pain, post-surgical pain, and phantom limb pain.
FES Center: Propelling the research forward
Investigators at different research stages share findings through FES collaboration, helping move discoveries toward clinical impact and eventual deployment.
“Science is not just about one person sitting in the corner thinking, ‘I have a brilliant idea.’ You need to bring people together,” Saab says.